If your previous child was born with a heart defect, it is completely natural to worry about this pregnancy. That worry is not irrational. It is a kind of careful thinking that can actually make a difference.
The honest answer is yes. A fetal echocardiogram is recommended in this pregnancy. But understanding why, and what it can and cannot tell you, is just as important as doing the test.
What is the actual risk?
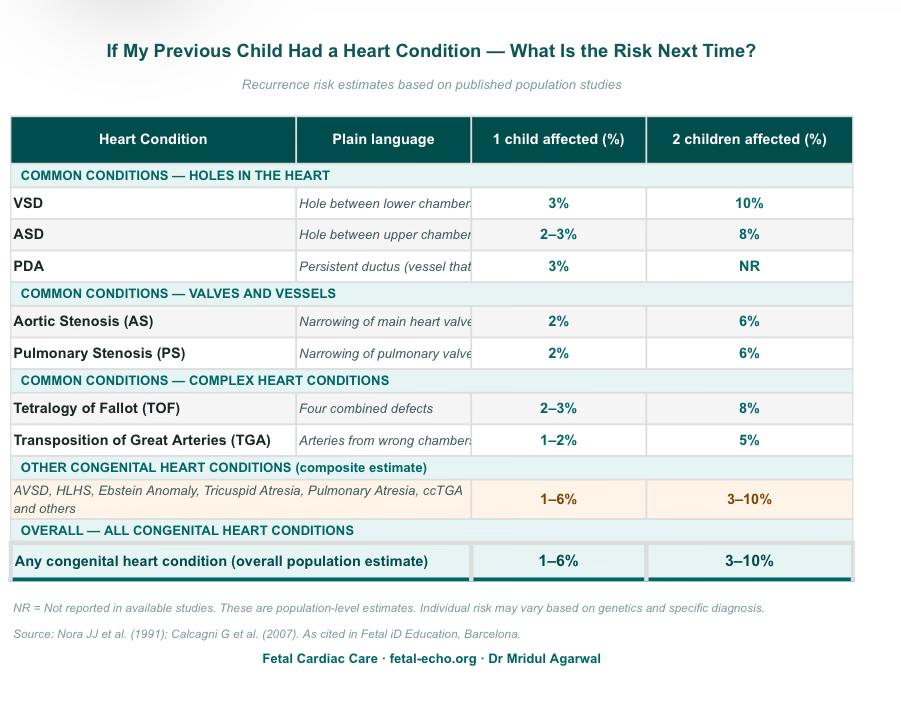
For most congenital heart defects, if one child in the family is affected, the chance of recurrence in the next pregnancy is roughly 2 to 4 percent. That is higher than the general population’s risk of around 0.8 percent, but it is still a relatively small number.
Some conditions carry a higher recurrence risk than others. Left heart obstructions, for example, tend to recur more often within families than simple septal defects. This is why a detailed assessment of what your first child had is an important part of planning this fetal echo.
What will the fetal echo look for?
The scan examines the structure of the baby’s heart in detail, including all four chambers, the valves, and the major vessels leaving the heart. It also looks at rhythm and function.
It is not a guarantee. No scan can detect every possible heart abnormality with certainty. But in experienced hands, a fetal echocardiogram detects the majority of significant structural heart defects, and it does so at a stage when there is still time to plan.
When should it be done?
The ideal window is between 18 and 22 weeks of pregnancy, when the heart is large enough to examine in detail. If there are strong reasons for concern, a preliminary scan can sometimes be done between 14 and 16 weeks, though a repeat at the standard window is usually recommended.
What if something is found?
A finding on fetal echo does not mean the same outcome as your previous experience. Heart defects exist on a wide spectrum. Some are mild and resolve without treatment. Others require careful monitoring, planned delivery, or early intervention after birth.
Finding something early gives your team time to prepare. That preparation changes outcomes.
What if nothing is found?
A normal fetal echo is genuinely reassuring. It does not eliminate all possible cardiac risk, but it significantly reduces it, and it means you can continue your pregnancy with much more confidence.
Here’s a shorter, gentle closing you can use:
In the end, a fetal echo is not just a test; it’s a way to replace fear with clarity. Whether it brings early answers or simple reassurance, it gives you back a sense of control. You’re doing what any caring parent does: choosing knowledge, choosing preparedness, and choosing peace for yourself and your baby.

